Summary
A LIMS for hospitals system makes lab operations digital and organized. When clinics integrate LIMS with EMR and HMS, the entire hospital gets connected. In traditional systems, hospitals lack connectivity. It took considerable time to generate lab reports. To overcome such complex practices, it is high time to adopt LIMS software. You cannot get enormous benefits from LIMS software alone. To further enhance the system usability, connect the software with the EMR and HMS modules. LIMS integration brings more connectivity among departments and makes the practices less stressful. In this blog, I will cover some interesting facts about LIMS integration with EMR and HMS and how it helps hospitals provide efficient and reliable services to patients. Keep reading!!
Introduction
In the modern healthcare system, laboratories play a crucial role. Blood tests, pathology reports, microbiology analysis, and diagnostic results are the base of patient treatment. If your lab operations are still depending on manual practices or different software, then clinics mostly face challenges with data delay, report errors, and workflow confusion. To combat such stressful scenarios, medical facilities should integrate a Laboratory Information Management System (LIMS) into the hospitals.
LIMS is a digital software system that automates all the complex functions of the laboratory. The biggest benefit of LIMS for hospitals integration with EMR and HMS is workflow efficiency and patient safety. Beyond that, hospital administration gets centralized dashboards that help easily monitor lab performance, test volumes, and operational metrics. LIMS integration is a strategic digital transformation step for hospitals. These integration systems help hospitals make better clinical decisions and reduce operational costs. Most importantly, LIMS-EMR-HMS integration helps clinics improve their services’ quality.
Why Do Hospital LIMS-EMR Integrations Fail after 2 years?
1. Understanding LIMS-EMR Integration as one-time IT project
Many hospitals consider LIMS integration a one-time IT project. Further, clinics should update and maintain software after the go-live stage, as lab tests and workflow needs keep changing with time and regulations. Therefore, it is crucial for clinics to update the system regularly.
2. Weak Governance and Ownership Problem
In many labs, there is no legitimate owner in the medical organization after the project is successfully completed. The clinic should hire a proper team to manage the integration. Further, many clinics lack a proper plan or roadmap and budget.
3. Fragile HL7 Interfaces and Customization Issues
Many times, clinics create integration from point-to-point HL7 mappings and quick customizations. Further, when vendors upgrade the software, they incorporate new features in the LIMS system. This integration easily gets broken, and clinics face challenges with data errors.
4. Poor Data Governance and Test Code Mapping Errors
The lab continues to add panels or test codes in the practices. Further, if clinics fail to map emr propely in the LIMS system, then results get saved in the incorrect location. In some cases, Lab Information System Software will display results in an unstructured format. This undermines the LIMS system’s credibility and trustworthiness.
LIMS for Hospitals: How to Avoid Common Traps in Integration?
1. Understanding Long-Term Support and Budget Planning
Clinics should have continuous technical support and a maintenance budget to run the clinics’ integration smoothly. Further, LIMS systems get outdated without proper funding and planning.
2. Follow Standards-Based Integration and Continuous Monitoring
Hospitals should use standards-based interfaces, regular monitoring, and alert systems. Further, this helps clinics detect bugs at an early stage. Integration remains stable and reliable for the long term.
How to Integrate LIMS with EMR/HMS using HL7 or FHIR standards?
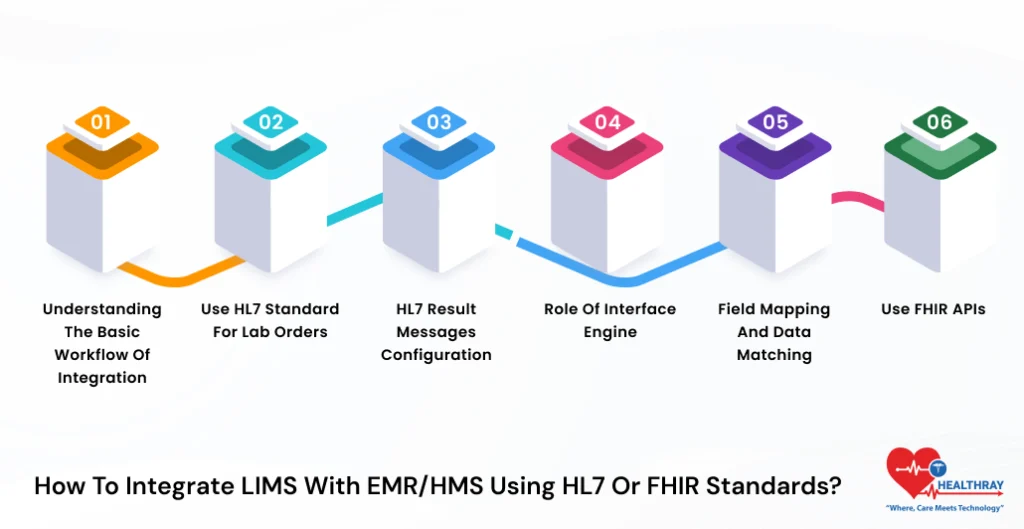
Let’s check out:
1. Understanding the Basic Workflow of Integration
Firstly, the lab should decide the data workflow. Usually EMR/HIS sends the lab orders to LIMS. Consequently, LIMS reverts the test results back to the EMR system.
2. Use HL7 Standard for lab orders
In HL7 v2 integration, lab software uses ORM (Order Message) to send orders to EMR. Further, this message contains patient details, test order and doctor information.
3. HL7 Result Messages Configuration
When lab tests get completed, Lab Solutions Software sends results to EMR through ORU (Observation Result Message). Further, it includes test values, reference range and report details.
4. Role of Interface Engine
To simplify the complex process of integration, hospitals use interface engines such as Mirth. Furthermore, thai system receives the mesages, convert it and sends them to different systems.
5. Field Mapping and Data Matching
It is highly paramount for clinics to map important fields at the time of integration. Further, clinics should properly map patient IDs, order codes, test names, results and reference ranges. A right mapping alleviates data errors that arise in the system.
6. Use FHIR APIs
FHIR is a modern standard that levages rest API to connect the systems. Further, it includes serviceRequest (orders), specimen, observation aur diagnostic report resources.
Step towards digital era with our healthcare solution
Revamp your hospital facilities and embrace change for better healthcare management. Ease in managing and organizing large medical datasets leads to effective analysis. Seize the opportunity now!
What are the Top Pitfalls of LIMS Projects?
1. Not Clear about Requirements and Goals
A common problem in LIMS projects arises when clinics do not have clear requirements and objectives for their practices. If clinics don’t put effort into writing clear documents of lab workflows, testing processes and reporting needs, then the LIMS system will not support real lab operations.
2. Not Considering Data Migration and Integration Effort
Few labs still think that transferring current data into a new LIMS system is simple. But in reality legacy data is messy and inconsistent. Clinics should first clean the patient records, test codes, and historical results and map them accurately in the LIMS software. Further, if the lab fails to perform proper validation and testing, then eventually data errors or missing records will pose many potential complications in the future.
3. Not Planning Realistic Budget and Timeline
Many organizations set unrealistic timelines and low budgets at the time of project planning. Further, lab management software implementation demands configuration, testing, integration and training. If realistic planning is not proper, the project will get subpar due to constraints. This will negatively impact the quality.
How Long Does it Take to Implement and Integrate LIMS in a Hospital Environment?
Hospital LIMS implementation timelines depend on project size and complexity. Let’s understand more about it:
1. Faster Implementation for Small Hospitals
If hospitals use cloud-based LIMS, then customizations are usually fewer. Further, the system gets deployed remarkably faster. Simple setups where workflow features and integration are limited take a few months. In many cases with preconfigured solutions, an active internal team, Lab, can achieve go-live in 6–12 weeks, or 30–90 days.
2. Longer timeline for Larger Hospitals
In large hospitals, clinics usually take 6-18 months for complete LIMS implementation. The reason behind this prolonged time is multiple lab departments, different analyzers, and complex EMR/HIS integrations. Further, legacy systems require extra time for data migration and regulatory validation.
3. Workflow Complexity Impact
Every lab has different workflows. Further, if the lab system requires multiple automations, it may take a long time for implementation. Sample tracking, reporting, and billing integration demand more time for configuration and testing.
4. Customization vs. Configuration
If a hospital system executes heavy customization, it may increase both time and cost. Further, Configuration-based approach is better, in which clinics adjust existing features to manage a workflow. This expedites the deployment and makes the maintenance processes easier. To fully comprehend, check out our blog’s LIMS ROI calculator.
What are the Main Benefits of Integrating LIMS with EMR/HMS for Patients and Clinicians?
1. Faster Lab Results Access for Doctors
When clinics integrate LIMS for hospitals with EMR/HMS integration, consequently, doctors get access to real-time patient lab records. Further, they no longer need to open different systems to extract patient reports from different departments. This is especially useful for emergency or critical care situations that require the fastest diagnosis and treatment decisions.
2. Improve Patient Safety and Quality of Care
In an integrated system, data are accurately accessed. Further, this minimizes the diagnostic errors and makes the care transition smooth. Hospitals can provide better monitoring and timely treatment that improves overall patient care.
3. Transparency and Engagement
Nowadays many hospitals use patient portals that are linked with EMR and HIS. Patients can view their lab results online, download reports and understand their health status more clearly. This allows patients to be involved actively in their healthcare journey.
How does LIMS Integration with EMR Actually Work End‑to‑End for Orders and Results?
Through EMR, doctors can conveniently place the lab orders for their patients. Further, doctors can check patient details, visit info and required tests. These orders are automatically generated in digital format. Once the order is received, LIMS assigns a unique specimen ID and generates barcode labels. These barcodes are useful for sample collection and tracking and avoid the risks of mismatches. LIMS for hospitals helps track lab inventory and sample usage in real-time, reducing wastage and avoiding delays. Let’s check further steps:
- LIMS tracks all the samples from collection to lab different sections and analyzers.
- Lab analyzers perform tests and directly send raw results to LIMS.
- Technologists and pathologists review the results and ensure everything is working as per protocols.
- Final validated results are resent to emr in HL7 ORU and FHIR formats.
- EMR matches the result with the original order.
- Doctors get real-time results and notifications.
Conclusion
Lab systems become patient-focused ecosystems when LIMS, EMR, and HMS are integrated. LIMS for hospitals integration makes the entire workflows connected and patient care becomes smooth and efficient. Integrated systems deliver more accurate tracking, audit trails and data management. Platforms such as Healthray assist clinics in strengthening their performance and patient outcomes.





