Quick Summary
If you’ve ever wondered why a hospital gets paid weeks after treating a patient, the answer lies in the medical billing process. It’s a detailed, step-by-step cycle that starts the moment a patient walks through the door and ends only when the final payment clears. Get any step wrong and the whole process slows down – or worse, the claim gets denied entirely. In this blog, we’ll walk you through all 10 steps clearly so you know exactly what’s happening at every stage.
Introduction
Let’s be honest – the medical billing process confuses a lot of people. Even experienced healthcare administrators sometimes struggle to explain what actually happens between a patient visit and a payment hitting the account. And that confusion costs hospitals real money every single day.
The medical billing process is the complete cycle of submitting and following up on claims with health insurance companies to receive payment for services a healthcare provider delivers. It sounds straightforward. However, in the real world, it is patient information, insurance cover, medical codes, claims forms, and tracking payments, all operating simultaneously. According to the estimates provided by the Centers for Medicare & Medicaid Services, there were a total of 28.83 billion Medicare Fee-for-Service improper payments in FY 2025, and the majority of them can be reduced to simple, preventable billing cycle errors.
This is precisely why the presence of the appropriate Medical Billing Software is so different. It keeps every step connected, reduces human error, and makes sure nothing falls through the cracks. It is with this in mind, that we will take a step-by-step look at each of the 10 steps, to understand where things are going to work, and where things are going to fail.
The 10 Steps In The Medical Billing Process – At A Glance
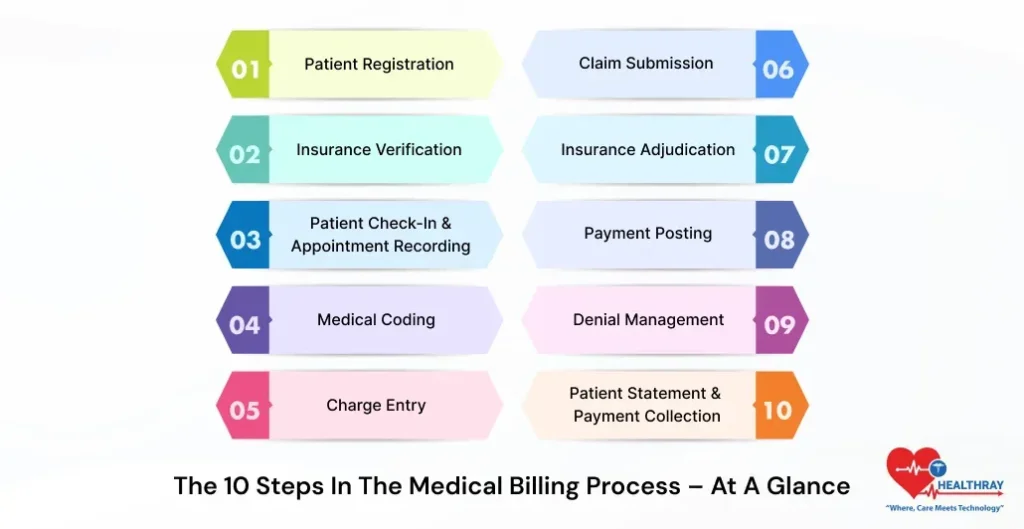
Before we dive into each step, here’s a quick overview of the full cycle:
- Patient Registration
- Insurance Verification
- Patient Check-In & Appointment Recording
- Medical Coding
- Charge Entry
- Claim Submission
- Insurance Adjudication
- Payment Posting
- Denial Management
- Patient Statement & Payment Collection
Now let’s break each one down properly..
Step 1 – Patient Registration
All the billing cycles begin with this one. And frankly speaking, in case you get this step wrong, the rest of it suffers due to it.
Registration of patients entails gathering of personal, demographic and insurance details of a patient during or prior to the initial visit. This will include full name, date of birth, address, contact details, insurance provider, policy number and group number. Even in the case of returning patients you have to check to ensure that all information that is available is current and correct, people switch insurance plans, change houses and contact numbers more frequently than you may assume.
The reason behind doing this is that it is basic. All the claims that you will present in the future will be based on this. One wrong character in a policy number or expired insurance card can result in disapproval of a claim some weeks down the line. And when it comes to locating the mistake in registration, it wastes everyone’s time.
Hospital medical billing software makes much of this step easy by ensuring that all the required fields are collected prior to the process. It also alerts on unfinished registrations yet it will be a billing problem in the future.
Pro Tip: Always collect a copy of the patient’s insurance card, front and back at every visit. Insurance details change more frequently than most practices expect, and a quick scan takes less than 30 seconds.
Step 2 – Insurance Verification
This is the point at which much of the billing issues begin and in which the appropriate process can avert most of the problems.
Insurance verification entails ensuring that the insurance cover of the patient is active, that your practice falls within the network of their insurance, and that the treatment or procedure the patient requires is actually covered. You would get surprised to see the number of patients who come to the assumption that they are covered in something which is not covered in their plan at all.
Moreover, there are also some specific treatments which cannot be prescripted without the prior consent of the insurance company. Failure to check this is one of the major causes of claims being denied in future. Indeed, the American Academy of Professional Coders discovered that the most common causes of claim denials in 2024 were preceding approvals and a lack of patient information in 2024 which can be prevented at this point.
Once completed correctly, insurance verification saves your billing department the time hassle of making follow-up calls on denials and the displeasant experience your patients get when told they must have to pay more. It is a 10-minute check which can save hours of rework.
Step 3 – Patient Check-In & Appointment Recording
After the patient arrives, the front desk checks him/her and the clinical team documents all the events during the visit. And we refer to everything.
The doctor records the chief complaint of the patient, physical examination, diagnosis, treatment plan, and procedures as well as medication that he or she has prescribed. The next step is the basis of medical coding on this documentation. Unless the notes are clear, complete or lack essential details, the coder is unable to give appropriate codes as well as the incorrect codes equate to the incorrect reimbursement.
Suppose that it were as follows, the more precise the clinical documentation, the more pure the downstream billing process. Good documentation habits in practices are continually associated with fewer claim rejections than poor documentation habits do.
When it comes to the case of patient records, which contain certified translation in particular in multilingual hospitals, it is also crucial that the translated records would not infringe on the required medical standards prior to entering the billing process. Errors in translating at this stage lead to coding issues which are difficult to diagnose, and expensive to fix.
Note: Many hospitals now use digital voice-to-text tools to capture physician notes in real time during consultations. This reduces documentation errors significantly and speeds up the coding process that follows.
Step 4 – Medical Coding
This is whereby the clinical language is translated in a way that the insurance companies can understand.
Medical coding involves the use of special alpha numerical codes to identify each diagnosis or procedure. Medical billing can be done in two types of codes, i.e. ICD-10 codes of diagnosis and CPT codes of procedures. There are over 70,000 ICD-10 codes and over 10,000 CPT codes. Here, accuracy is required.
One misplaced code can modify the whole claim. As an example, when the normal consultation is billed as a complex consultation or the wrong procedure does not get coded, this may lead to either underpayment or even an allegation of fraud. None of these is what is desired.
The number one causes of non-payment claims included prior authorizations and missing information about the patient in 2024. All these cannot be avoided during the insurance verifications.
Step 5 – Charge Entry
After the assignment of the codes, the billing team determines the total charges of the visit and key-in them in the billing system.
Charge entry implies everything; a list of all services, procedures and supplies that were involved in the visit of the patient, in addition to the appropriate billing codes and appropriate costs. Every service has its line item, everything is not bundled or omitted. The medical billing software will then ensure that all the codes are matched with the charge associated with them and throws a warning on any misfits prior to the claim processing ahead.
It is a more critical step as it may seem. Undercharging translates into a loss of revenue that is rightfully enjoyed in the hospital. Even being inadvertent about overcharging will attract an audit. It means that to be able to enter the charges right, one needs not only accuracy but also an in-depth knowledge of your price list.
Step 6 – Claim Submission
Once charge entry is complete, the claim is ready to go to the insurance company. However, it does not simply get posted and that is something that many people are not aware of.
Most claims go through a clearinghouse first. Think of a clearinghouse as a middleman that checks your claim for errors before it reaches the payer. It validates that all fields are complete, codes are correct, and the format meets the insurer’s requirements. Various payers have varying formatting needs and a clearinghouse takes care of this translation.
Claims can be submitted electronically or on paper, but electronic submission is now the only practical option. It’s faster, more accurate, and most insurance companies process electronic claims significantly quicker than paper ones. Research shows that nearly one in five in-network claims gets denied which is exactly why a structured denial management process isn’t optional anymore..
It is also the time when your medical services documentation should be airtight. Every service billed must match the clinical notes from the visit. Any difference between what was written and what was billed raises eyebrows on the part of the insurance adjudicator to whom the claim is presented.
Step 7 – Insurance Adjudication
This process is handled entirely by the insurance company, where your claim is approved, adjusted, or denied.
Adjudication is the process where the insurance company reviews your claim and determines the payment amount. They verify patient coverage, medical necessity, provider network status, and that codes match documented services. It is comprehensive since it sounds comprehensive.
The outcome of adjudication falls into one of three categories. The claim is fully paid, partially paid or rejected. A partial payment usually means the insurance company covered their portion and the remainder becomes the patient’s responsibility. A denial implies that the claim is returned with an explanation of the reasons why payment has been rejected.
And here’s the thing, denials aren’t always final. Many of them are fixable. You must do it quickly though since most insurance companies are very strict on resubmissions and appeals. Without that window, one loses the payment entirely.
Step 8 – Payment Posting
Once the insurance company processes the claim, they send back an Explanation of Benefits commonly called an EOB. Posting the payment involves recording the payment correctly in your billing system.
This is a step more detailed than it may sound. Billing must reconcile all payments with the initial claim and identify any discrepancies immediately. Confirm the amount received matches the expected payment for each claim. If insurance pays less than anticipated, determine whether to bill the patient or contest the claim.
Proper payment posting provides your practice with a current view of its financial condition. It also leaves behind an audit trail that is clean and that is of great significance in case a claim is ever challenged in future. Sloppy payment posting causes revenue leakage that is actually hard to track back and recover.
Step 9 – Denial Management
Let’s be straightforward about this claim denials are a normal part of the medical billing process. All practices are concerned with them. The difference between financially healthy practices and troubled practices is the rate at which they handle those denials.
Denial management is a process of reviewing all denied claims, finding out the cause of the denial, rectifying the problem and submitting the claim again within the deadline of the payer. Common denial reasons include incorrect patient information, missing prior authorisation, coding errors, duplicate claims, and services not covered under the patient’s plan.
The key is to monitor the trends of denial. When the same form of denial continues to occur, it is an indicator of a widespread issue somewhere in the previous stages of registration, verification, coding, or charge entries. It is much more effective to fix the problem upstream rather than deny the individual denials one at a time.
Types of Medical Billing Software vary significantly in how they handle denial management. Some systems flag potential denial risks before a claim is even submitted – which is the level of intelligence your billing team genuinely needs to stay ahead of rejections.
Step 10 – Patient Statement and Payment Collection
After insurance pays their portion, whatever remains becomes the patient’s financial responsibility. This last action has to do with communicating that balance effectively and gathering it effectively.
The patient statement should clearly show what services were provided, what the insurance paid, and exactly what the patient owes. The second largest cause of delays in payment or even disagreement of payment by patients is confusing or vague statements. Clear and plain language statements with various payment options; online, phone, in person make a real difference to collection rates.
Follow-up is also important here. Not all patients make immediate payments. An organized follow-up program – automatic reminders, payment plans and friendly yet firm communications keep your accounts receivable out of bad debt. The more time a balance remains unpaid the more difficult it is to collect.
Why The Right Medical Billing Software Changes Everything
This is one thing that is worth saying as long as the medical billing process itself is as strong as the system that drives it. The system is slow, prone to errors and costly in terms of manual billing in all the 10 steps. And it is a risk that no practice should take in the current healthcare environment.
The right [medical billing software] integrates all the cycles on a platform. Insurance verification is fed off patient registration. Coding feeds off of clinical notes. Codes feed into charge entry. Claims submit automatically. Denials are flagged on-the-fly. Payments post accurately. Patient statements go out on schedule. There are no gaps in the cracks since all remains interrelated.
Healthray’s medical billing solution is built specifically for hospitals and healthcare practices that need this kind of end-to-end control. It reduces claim rejection rates, speeds up reimbursement timelines, and gives your billing team the clarity they need to stay on top of every claim from submission to payment.
To put it simply, the right software doesn’t just make billing easier. It makes your entire revenue cycle healthier.
Conclusion
The medical billing process isn’t just an administrative function it’s the financial backbone of every healthcare practice. Get it right and your cash flow stays healthy, your staff works efficiently, and your patients trust the billing experience. Get it wrong and the consequences ripple through every department.
Each of the 10 steps plays a specific role in making sure that the care your team delivers translates into accurate, timely payment. From patient registration all the way to final payment collection, every step deserves attention and the right tools to support it. And honestly most billing problems don’t come from bad staff. They come from disconnected systems and manual processes that were never built for today’s volume and complexity.
If your current billing process feels chaotic, inconsistent, or slow, the answer usually isn’t more people. It’s a smarter system that connects every step automatically and catches errors before they become denials.
That’s exactly what Healthray’s medical billing software is built to do. If you’re curious about how it works for practices like yours, you can start free and explore it at your own pace – no pressure, no commitment, no sales call unless you want one.
Learn more:All You Need To Know About Medical Expense Tracking Software





